Causes of Foot Stress Fractures
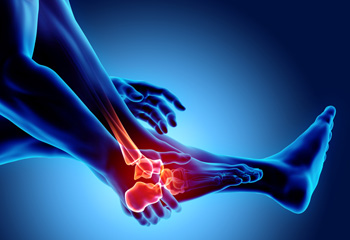
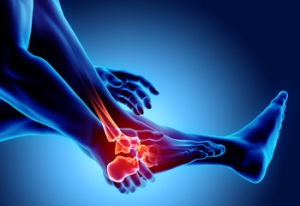
A foot stress fracture, a condition prevalent among athletes and individuals engaged in repetitive weight-bearing activities, is characterized by tiny cracks in the bones of the foot. These fractures often result from overuse, with excessive and repetitive impact on the feet causing structural fatigue. Contributing causes include sudden increases in physical activity, improper footwear, or inadequate training surfaces. Symptoms manifest gradually, beginning with localized pain during activity that subsides with rest. As the stress fracture progresses, the pain becomes persistent, and swelling may occur. Tenderness to touch, particularly at specific points on the foot, is a common indicator. Ignoring these symptoms can lead to more severe fractures, potentially requiring prolonged recovery. Understanding the definition, causes, and symptoms of foot stress fractures is essential for individuals engaged in high-impact activities. If you have a foot stress fracture, it is suggested that you make an appointment with a podiatrist who can guide you toward the best treatment.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Dan Kirk, DPM from Bluffton Foot & Ankle. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our offices located in Bluffton and Celina, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
Definition and Symptoms of Plantar Fasciitis
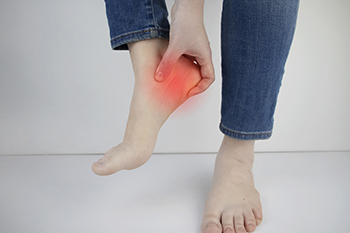
Plantar fasciitis is a common foot ailment characterized by inflammation of the plantar fascia, a thick band of tissue that connects the heel bone to the toes. The condition typically results from repetitive strain or excessive stress on the feet, causing tiny tears in the ligament. Individuals with plantar fasciitis often experience a stabbing pain near the heel, especially with the first steps in the morning. This discomfort may gradually subside during the day, only to resurface after prolonged periods of standing or intense physical activity. The pain tends to be more pronounced after sitting for an extended duration and can impact daily activities, affecting the overall quality of life. Understanding the definition and recognizing the symptoms of plantar fasciitis is essential for timely intervention and management. Plantar fasciitis can cause severe pain and discomfort. If you have developed this condition, it is strongly suggested that you are under the care of a podiatrist who can guide you toward the correct treatment method.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dan Kirk, DPM from Bluffton Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our offices located in Bluffton and Celina, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Foot Pain May Indicate PAD
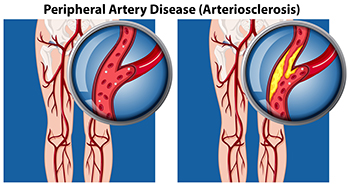
Foot pain is more than just an annoyance. It can signal a potential threat to your overall health. One such condition linked to foot discomfort is peripheral artery disease, abbreviated PAD, and is a serious condition that, if left untreated, can have fatal consequences. PAD occurs when fatty deposits accumulate in the arteries, restricting blood flow to the leg muscles. This condition is not to be taken lightly, as it often leads to more severe complications, such as coronary heart disease and an increased risk of strokes. Recognizing the signs of PAD early on is essential for effective treatment and prevention of further complications. The primary indicators of peripheral artery disease are recurring leg pain during exercise, foot pain, persistent ulcers, and the development of gangrene. Foot pain, ranging from mild to severe, is a common symptom that typically subsides with rest. If you notice open sores, known as ulcers, on your feet or legs that do not heal, it is essential to consult with your podiatrist promptly. Gangrene, a severe condition characterized by swelling, pain, and the production of foul-smelling pus, can occur when PAD progresses. Skin changes, such as coldness, numbness, and discoloration, may also manifest. If you are experiencing symptoms of peripheral artery disease in the feet and ankles, it is suggested that you schedule an appointment with a podiatrist for treatment.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dan Kirk, DPM from Bluffton Foot & Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
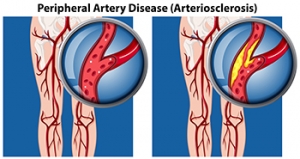
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our offices located in Bluffton and Celina, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Peripheral Artery Disease
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
Surgery Considerations for Plantar Fibroma
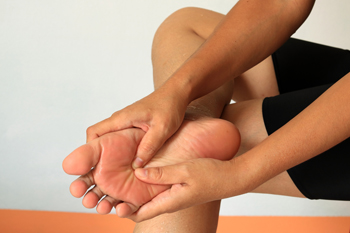
Plantar fibroma, a benign yet often painful growth on the sole of the foot, presents challenges that prompt a range of treatment options. Non-surgical approaches typically involve conservative methods, such as orthotics and corticosteroid injections, to alleviate symptoms and reduce inflammation. However, in cases where the fibroma causes persistent discomfort or interferes with daily activities, surgical intervention may be considered. Surgery for plantar fibroma aims at excising the fibrous tissue and restoring optimal foot function. The procedure involves careful consideration of the fibroma's size, location, and impact on surrounding structures. Recovery from surgery may involve a period of immobilization to regain strength and flexibility. While surgical intervention poses inherent risks, it can offer significant relief and improved mobility for individuals grappling with the challenges posed by a plantar fibroma. If you have developed a plantar fibroma, it is suggested that you consult with a podiatrist who can determine if surgery is a correct treatment option for you.
A plantar fibroma may disrupt your daily activities. If you have any concerns, contact Dan Kirk, DPM of Bluffton Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Plantar Fibroma
A plantar fibroma is a fibrous knot in the arch of the foot. It is embedded in the plantar fascia which is a band of tissue that extends from the heel to the toes along the bottom of the foot. There can be multiple plantar fibromas in the feet at the same time. There are no known causes for this condition. If you have a plantar fibroma, there will be a bump in the arch of your foot that cannot be missed. Any associated pain is most often due to a shoe rubbing against the nodule. Non-surgical options, such as steroid injections, physical therapy, and orthotics should be tried first. Surgery is a last resort and is the only thing that will remove a plantar fibroma entirely. Consult with a podiatrist for a proper diagnosis and to determine the treatment regimen that is right for you.
What Causes a Plantar Fibroma?
While there are no specific causes identified, a plantar fibroma can possibly come from genetic predisposition or the formation of scar tissue that forms from healing the tears in the plantar fascia.
What Are the Symptoms of a Plantar Fibroma?
There will be a noticeable lump in the arch of the foot that may or may not cause pain. If pain is felt, it is typically because a shoe is rubbing up against the lump or when walking or standing barefoot.
Treatment and Prevention
A plantar fibroma will not disappear without treatment, but it can get smaller and be a non-issue. If pain persists, a podiatrist examines the foot and when the arch of the foot is pressed, pain can be felt down to the toes. An MRI or biopsy might be performed to help diagnose or evaluate the plantar fibroma. The following non-surgical options are generally enough to reduce the size and pain of these nodules:
- Steroid injections
- Orthotics
- Physical therapy to help apply anti-inflammatory creams on the bump
Surgery is considered if the mass increases in size and the patient continues to feel pain after non-surgical methods are tried.
If you have any questions please feel free to contact our offices located in Bluffton and Celina, OH . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Plantar Fibroma
A plantar fibroma is a knot in the arch of the foot. It can cause pain when repeated pressure is applied by walking barefoot or wearing tight shoes. While plantar fibromas can appear in anyone, men who are middle-aged or older are said to be more susceptible. The main symptom of a plantar fibroma is a firm lump on the arch of the foot. If there is pain, it can be intensified by putting pressure on the nodule. The lump can stay one size or grow larger. You may have one or more fibromas in the feet and there tends to be a high incidence of recurring plantar fibromas. Generally, a plantar fibroma can be treated without surgery. Treatment might include steroid injections to help shrink the lump, orthotics to help redistribute weight away from the nodule, plantar fascia stretching, or physical therapy to help use anti-inflammatory medication on the lump. If a lump grows larger or more painful, a podiatrist can be consulted to confirm the diagnosis. The doctor will palpate the lump and this may cause pain that can be felt all the way to the toes. An X-ray, MRI, or biopsy might be done if further evaluation is necessary. A lump in the arch of the foot might be something other than a plantar fibroma, such as cysts, nerve or fatty tumors, swollen tendons, or an infection in the foot. It is important to see a podiatrist for proper diagnosis and treatment of plantar fibromas.
Is It a Good Idea to Run In Walking Shoes?

Many people wonder whether it is acceptable to run in walking shoes. While walking shoes are designed for a different purpose than running shoes, the answer is not always a straightforward yes or no. Walking shoes are generally built with a focus on providing comfort, stability, and support during low-impact activities like walking. They often have less cushioning and flexibility compared to running shoes, which are designed to absorb the higher impact forces generated during running. For short, light jogging or occasional runs, walking shoes may suffice, especially if you do not experience discomfort or pain. However, if you plan to run regularly or for longer distances, investing in running-specific footwear is recommended. Running shoes offer the necessary cushioning, shock absorption, and flexibility designed to protect your feet and joints from the impact of running. Ultimately, choosing the right footwear depends on your activity level and goals. If you are serious about running, it is best to invest in a proper pair of running shoes to reduce the risk of injury and enhance your performance. If you would like additional information about walking and running shoes, it is suggested that you confer with a podiatrist who can provide you with the knowledge you are seeking.
For more information about walking shoes versus running shoes, consult with Dan Kirk, DPM from Bluffton Foot & Ankle. Our doctor can measure your feet to determine what your needs are and help you find an appropriate pair of footwear.
Foot Health: The Differences between Walking & Running Shoes
There are great ways to stay in shape: running and walking are two great exercises to a healthy lifestyle. It is important to know that running shoes and walking shoes are not interchangeable. There is a key difference on how the feet hit the ground when someone is running or walking. This is why one should be aware that a shoe is designed differently for each activity.
You may be asking yourself what the real differences are between walking and running shoes and the answers may shock you.
Differences
Walking doesn’t involve as much stress or impact on the feet as running does. However, this doesn’t mean that you should be any less prepared. When you’re walking, you land on your heels and have your foot roll forward. This rolling motion requires additional support to the feet.
Flexibility – Walking shoes are designed to have soft, flexible soles. This allows the walker to push off easily with each step.
If you have any questions, please feel free to contact our offices located in Bluffton and Celina, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.